Melanoma is malignant and very aggressivea skin tumor that develops as a result of melanocytes and melanoblasts regenerating - the pigment cells producing the pigment melanin. The tumor contains a large amount of melanin in its cells - this is the reason for the dark color. But sometimes there are variants without a pigment. Of all skin tumors, only 10% is melanoma. Recently, there has been a continuous increase in the incidence rate in this area. The number of diagnoses of skin melanoma over the past decades has grown at times. It is noted that at the age of sixty years both women and men fall ill with the same frequency. On the age range of thirty to fifty years, the peak incidence. Those who already have melanoma, the risk of a new one - about twelve percent. In this disease, the prognosis is extremely unfavorable - in the structure of mortality, melanoma of the skin is in the ninth place (1% of patients with malignant tumors die from melanoma).
The causes of melanoma
For melanoma, the main reason -exposure to ultraviolet radiation on exposed unprotected skin. Ultraviolet irradiation has a carcinogenic character, especially it is traced in squamous and basal cell carcinoma of the skin. For the development of skin melanoma, much will mean the intensity. Most often, melanoma occurs precisely as a result of a single ultraviolet irradiation with a high intensity. It can develop in those patients who have received sunburns in childhood or adolescence, often the occurrence of it in people who spend most of their time indoors and go on vacation to hot countries. In the development of melanoma, a significant role can be played by the trauma of the already existing nevus pigmentosa. But it can not be ruled out that, due to trauma, the tumor does not begin to grow, but only accelerates development, since it originated long before that. This can be a single exposure to nevi - a bruise, a cut, an abrasion - or a chronic effect: rubbing with chains, stiff details, seams of clothing, etc. Many scientific researches are devoted to the study of heredity in the etiology of the tumor. For example, it is established that in those families where there is a dysplastic nevus syndrome, there is an increased incidence of melanoma of the skin. Those who have this syndrome, throughout life, can develop a variety of dysplastic nevi - their number may be more than 50 with a very high risk of degeneration in melanoma. In this syndrome, the type of inheritance is autosomal dominant. Therefore, when making a diagnosis, all relatives who are close relatives should be sent to the oncologist for an examination. It is highly desirable that such patients apply to the oncologist for a checkup every six months to promptly identify the signs of the disease. Increasingly, much attention was paid to immune factors in the development of a disease such as skin melanoma. Immunodepression, as well as immunodeficiency states, are factors that contribute to the onset of this disease. It has also been established that hormonal status affects the development of melanoma of the skin, in particular this is seen in relation to women. To impart malignancy to existing pigment nevi can have a stimulating effect of puberty, menopause, pregnancy. 
Classification of melanoma, stage
There are four stages in the development of melanoma:
- the first stage: melanoma up to 2 mm thick, regional and distant metastases are absent.
- the second stage - melanoma more than 2 mm thick, there are no regional and distant metastases.
- the third stage - it is exposed when the lymph nodes are damaged.
- The fourth stage is set if distant metastases are detected.
Melanoma most often metastasizes to the liver andlungs. Possible damage to the skin, bones of the skeleton, brain. With visceral metastases, the prognosis can be extremely unfavorable, life expectancy can be on average six months. According to the prevalence and histological variant, melanoma can be divided into three main forms:
In addition, you should know that in addition to the surfaceskin melanoma can occur in the vascular membranes of the eyes, under the nail plates, on the mucous membranes (nasal cavity, conjunctiva, rectum mucosa, vagina), on the scalp. Such localizations, however, are very rare. 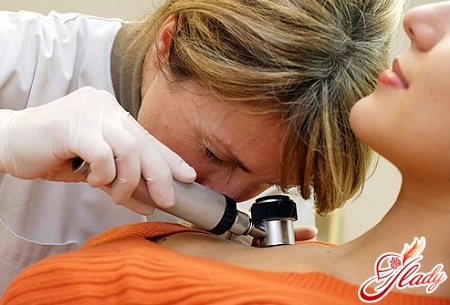
Diagnosis of the disease
Despite the availability of melanoma for examination, ina correct diagnosis can be difficult. Sometimes it is impossible to distinguish melanoma from a pigment nevus, and a careful attitude to a conversation with a patient can be of great importance for setting the right diagnosis. If there are suspicions of melanoma, it is necessary to conduct a morphological study. The final diagnosis can be established with his help. Cytological examination is performed in the presence of ulceration - from the surface of the tumor take smears. In case of doubt in the diagnosis, the main way to establish the correct picture is an excisional biopsy (it assumes complete excision of the tumor with a deviation of 2-5 mm from its edges), immediately after which a histological conclusion should be made. If the diagnosis is confirmed, a wide excision should be performed immediately. A biopsy should be performed under general anesthesia, when piercing the melanoma zone needle, it is possible that the tumor cells spread to the surrounding tissue. To assess the spread of the tumor process, if melanoma is already established, ultrasound should be performed for lymphatic regional nodes, chest X-ray, ultrasound of the abdominal cavity organs.
Symptoms of melanoma
A competent doctor is well versed inpathological elements and neoplasms on the surface of the skin, but for the average person the pigment changes will for the most part seem like a mole. In order not to miss the appearance of melanoma, it is necessary to know some symptoms, characteristic features of this disease. The first symptoms and signs of skin melanoma include:
- the change in tumor size is slow growth.
- the tumor can acquire a convex shape.
- The color changes, unevenly colored areas appear.
- the outlines change, appear rugged, irregular edges.
- asymmetry.
- bleeding, the appearance of crusts.
- itching, the sensitivity changes in the tumor area.
The most common complaints are patientsthe appearance of pigmented formation or an increase in the already existing in size, itching and burning in the area of the tumor, bleeding appears. Melanoma symptoms can be both basic and additional. Additional signs include a lack of skin pattern, hair loss at this place, skin peeling, the appearance of seals on the surface of the tumor. The lymph nodes nearest the tumor may increase. 
Prevention of melanoma
To prevent melanoma,limit stay in the sun. If a person is at risk, use sunscreen products that have a protection factor of at least 15, wear light, closed clothing, and always wear a hat. Some of the types of melanomas have a hereditary predisposition, so in the event that relatives have ever been diagnosed with melanoma, a checkup should be performed regularly at the dermatologist.
How to treat melanoma
Melanoma skin is mostly treated withsurgical methods. This applies to both the primary foci and to metastases in lymphatic regional nodes. Other treatments, which include radiation therapy, chemotherapy, immunotherapy, can not be considered an alternative to surgical intervention. But these methods can find their application in the case of a common tumor process, with the appearance of distant metastases. Treatment of melanoma - 1-2 stage Treatment of skin melanoma by surgical methods should be performed under general anesthesia in a specialized oncology unit. Early detection of melanoma and timely excision is the basis for successful treatment, the result of which can be a complete escape from a dangerous ailment. Radical intervention is understood as the excision of the tumor with the entrapment of the surrounding skin, subcutaneous fatty tissue under it, fascia or aponeurosis. The smallest spacing from the edge of the tumor can be 1 cm. After excision of melanoma, it is not always possible to eliminate the defect simply by reducing the edges of the wound. Various types of plastic substitution can be performed - for example, plastic using a free skin flap, local tissues, transplantation of flaps with an axial type of blood supply is possible. Treatment of melanoma: the third stage After excision of melanoma, the disease often continues to progress. Most often this is manifested by metastases of regional lymph nodes, which patients can detect independently or it becomes clear with ultrasound. Lymphatic collectors are mainly located in the axillary, inguinal areas. To confirm the diagnosis, a fine needle biopsy is performed for the enlarged lymph node. If melanoma cells are found, the entire lymphatic system in this area is removed, a single unit with surrounding fiber. The operation refers to traumatic, in the postoperative period it is often accompanied by lymphatic drainage, that is, lymphatic drainage. In the cavity of the wound, drainage should be installed - a hollow tube of rubber, which will facilitate the outflow of lymph from the wound cavity. In the postoperative period, it is possible to conduct additional methods of treatment - chemotherapy, radiation therapy. Treatment of stage 4 melanoma Despite the unfavorable prognosis, it is possible to perform treatment for this category of patients in order to prolong life, for which a variety of modern methods are used. As indications for surgical intervention can be identified:
- removal of a single metastasis, if there are no other lesions, and the patient's general condition is good;
- elimination of symptoms that significantly reduce the quality of life of the patient or threaten life.
- decrease in tumor mass to increase sensitivity to chemotherapy.
Chemotherapy for melanoma
Treatment of melanoma with chemotherapyapply when patients have distant metastases. To achieve stabilization of the process using modern chemotherapy schemes is possible only in twenty percent of cases, that is, the efficiency is rather low because of the low sensitivity of melanoma to the drugs. In the case of a common tumor process, radiation therapy may be used. It is used mainly in the presence in the brain of distant metastases or localized damage to bones. The effectiveness of this method is much inferior to surgery, so the indications for this method of treatment are limited.